Introduction
Welcome to the world of vital signs monitoring! A vital signs monitor is a crucial tool used in healthcare settings to assess a patient’s overall health and wellbeing. It provides real-time measurements of key physiological parameters, enabling healthcare professionals to quickly identify any potential abnormalities or changes in a patient’s vital signs.
Whether you’re a healthcare professional, a student studying healthcare, or simply a curious individual interested in learning more, this article will guide you through the basics of reading a vital signs monitor. By understanding how to interpret the various readings and recognizing any abnormalities, you’ll be better equipped to provide optimal care and support to patients.
Throughout this article, we’ll delve into the fundamental aspects of a vital signs monitor and explore the significance of heart rate, blood pressure, respiratory rate, and oxygen saturation levels. We’ll also discuss how to recognize and respond to alarms and troubleshoot common issues that may arise during monitoring.
Before we embark on this journey, it’s important to note that while reading a vital signs monitor is a valuable skill, it’s essential to rely on your clinical judgment and consult healthcare professionals for appropriate assessment and treatment. This guide aims to provide a foundation of knowledge and understanding, but it is not a substitute for proper medical training.
Now, let’s dive into the world of vital signs monitoring and begin our exploration of how to effectively read and interpret the data displayed on a vital signs monitor.
Understanding the Basics of a Vital Signs Monitor
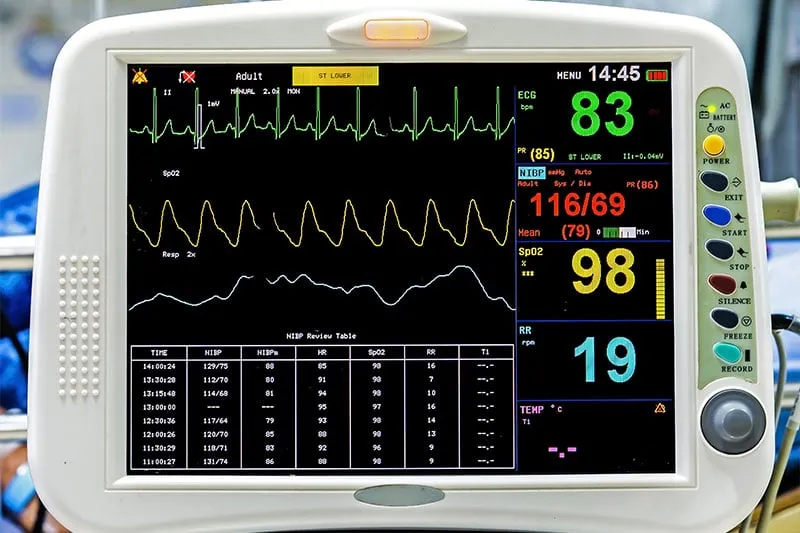
A vital signs monitor is a sophisticated medical device that measures and displays various physiological parameters essential for assessing a patient’s overall health. It typically consists of multiple components, including a monitor display screen, sensors, cables, and sometimes additional devices such as a blood pressure cuff or pulse oximeter.
The monitor display screen acts as the central hub, providing real-time data and vital sign readings. The sensors, strategically placed on the patient’s body, capture and transmit the necessary information to the monitor. These sensors can detect and measure different vital signs, including heart rate, blood pressure, respiratory rate, and oxygen saturation levels.
Heart Rate: The heart rate reading indicates the number of times the heart beats per minute (bpm). It is a key indicator of cardiac function and overall cardiovascular health. The normal range for adults is typically between 60 and 100 bpm. A higher heart rate may indicate factors such as exercise, stress, or an underlying medical condition, while a lower heart rate may be a sign of bradycardia or certain medications.
Blood Pressure: Blood pressure is measured in millimeters of mercury (mmHg) and consists of two values: systolic pressure and diastolic pressure. The systolic pressure represents the force exerted on the arterial walls when the heart contracts and pumps blood. The diastolic pressure is the pressure in the arteries when the heart is at rest between beats. A normal blood pressure reading for adults is typically around 120/80 mmHg. Abnormalities in blood pressure may indicate hypertension (high blood pressure) or hypotension (low blood pressure).
Respiratory Rate: The respiratory rate is the number of breaths taken per minute. It is an essential parameter indicating lung function and respiratory health. The normal range for adults is usually between 12 and 20 breaths per minute. An increased or decreased respiratory rate may be a sign of various respiratory conditions, pain, anxiety, or medication side effects.
Oxygen Saturation: Oxygen saturation levels, often referred to as SpO2, represent the percentage of oxygen-bound hemoglobin in the blood. It provides insights into the patient’s oxygenation status. The normal range for SpO2 is typically 95% and above. A lower oxygen saturation level may indicate hypoxemia, which can be caused by respiratory problems, heart conditions, or other factors.
Understanding these basic parameters is vital to effectively read a vital signs monitor. By familiarizing yourself with their normal ranges and the significance of any deviations, you can quickly identify potential abnormalities and take appropriate actions to ensure patient well-being.
Interpreting Heart Rate Readings
Heart rate is a vital parameter that provides valuable information about the cardiovascular health of an individual. Interpreting heart rate readings correctly is essential for detecting abnormalities and assessing a patient’s overall well-being. Let’s explore how to interpret heart rate readings on a vital signs monitor.
The heart rate is measured in beats per minute (bpm), reflecting the number of times the heart contracts and pumps blood. The normal range for adults is typically between 60 and 100 bpm. However, it’s important to note that heart rate can vary depending on multiple factors, including age, physical activity, stress levels, and any underlying medical conditions.
When interpreting heart rate readings, it’s crucial to consider the context and the patient’s individual characteristics. For example, a lower heart rate than the normal range, known as bradycardia, may indicate various factors such as athletic conditioning, certain medications (beta-blockers), or an underlying medical condition. On the other hand, a higher heart rate, known as tachycardia, may be a response to exercise, stress, fever, pain, anxiety, or underlying conditions such as arrhythmias or heart failure.
Additionally, it’s important to observe any significant changes in heart rate over time. A sudden increase or decrease in heart rate may signal an acute issue or a deteriorating condition. These changes should be closely monitored and evaluated by healthcare professionals to determine the appropriate course of action.
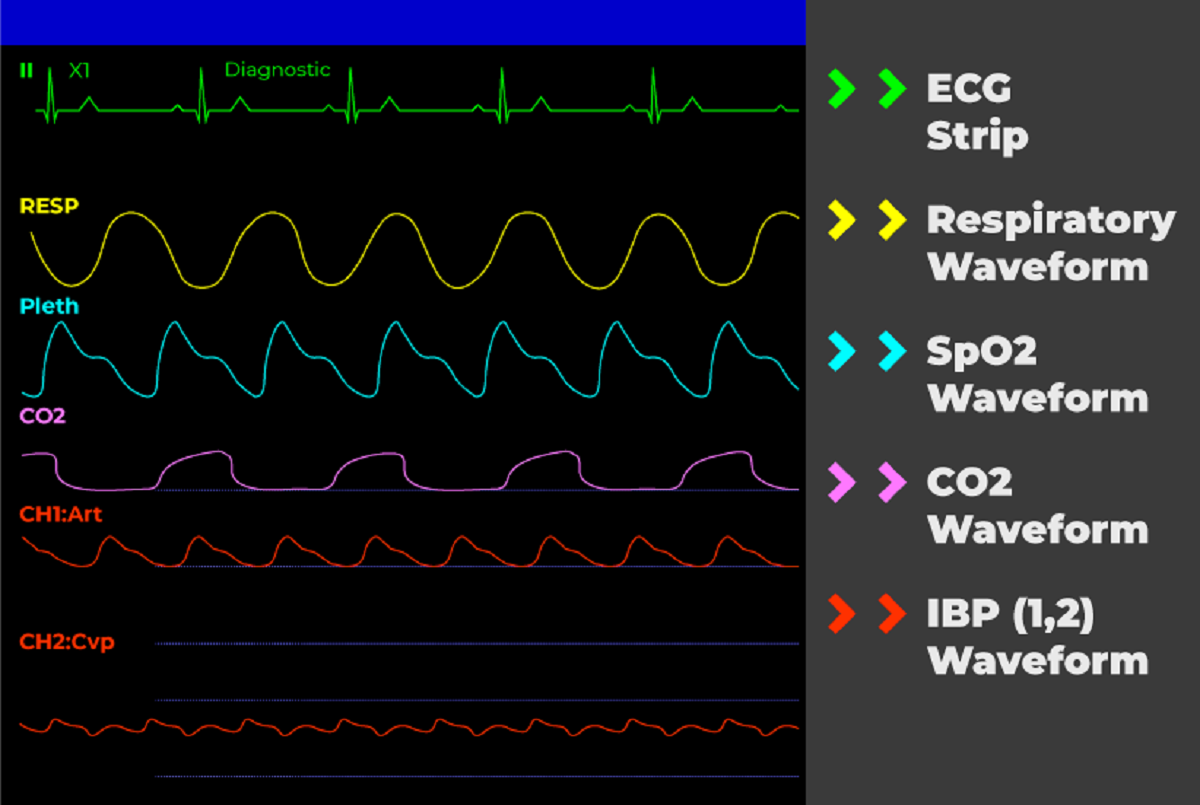
In certain cases, a vital signs monitor may also display other parameters associated with heart rate, such as rhythm and waveform. These can provide further insights into the heart’s electrical activity and help identify potential irregularities or abnormalities.
Rhythm: The rhythm of a heartbeat refers to the regularity and pattern of the heart’s contractions. A normal sinus rhythm indicates a regular and consistent heartbeat. Any irregularities in the rhythm may suggest an arrhythmia, which could be benign or require further investigation.
Waveform: The waveform displayed on the monitor represents the electrical activity of the heart, known as an electrocardiogram (ECG or EKG). In addition to heart rate and rhythm, the waveform can reveal abnormalities such as atrial fibrillation, ventricular tachycardia, or other cardiac dysfunctions.
Interpreting heart rate readings requires a combination of understanding normal ranges, considering the patient’s unique factors, and recognizing patterns or abnormalities in rhythm and waveform. Monitoring closely and consulting healthcare professionals when necessary ensures accurate assessment and appropriate intervention for the patient’s cardiac health.
Analyzing Blood Pressure Measurements
Blood pressure is a critical indicator of cardiovascular health and plays a crucial role in assessing a patient’s overall well-being. Analyzing blood pressure measurements accurately is essential for identifying abnormalities and monitoring changes in a patient’s condition. Let’s delve into the process of analyzing blood pressure readings on a vital signs monitor.
Blood pressure is measured in millimeters of mercury (mmHg) and consists of two values: systolic pressure and diastolic pressure. Systolic pressure represents the force exerted by the heart when it contracts and pumps blood, while diastolic pressure reflects the pressure in the arteries when the heart is at rest between beats.
A normal blood pressure reading for adults typically falls around 120/80 mmHg, where 120 represents the systolic pressure and 80 represents the diastolic pressure. Deviations from this range can indicate underlying health issues or other factors affecting blood pressure.
When analyzing blood pressure measurements, it’s important to consider both values in relation to each other. An elevation in systolic pressure, known as systolic hypertension, may be indicative of factors such as hypertension, stress, obesity, or artery stiffness. Elevated diastolic pressure, known as diastolic hypertension, could point to conditions like hypertension, kidney problems, or certain medications.
Conversely, low blood pressure, also called hypotension, can occur due to various reasons, such as dehydration, bleeding, medication side effects, or underlying medical conditions. It is important to monitor blood pressure consistently and consider the patient’s overall clinical presentation to determine the appropriate response.
Moreover, analyzing trends and changes in blood pressure measurements over time is vital in understanding the patient’s condition. Careful examination of recurring patterns, such as consistent hypertension or fluctuating blood pressure, can provide valuable insights into an individual’s overall cardiovascular health and help guide treatment decisions.
In addition to systolic and diastolic pressure, a vital signs monitor may also display other blood pressure-related parameters, including mean arterial pressure (MAP) or pulse pressure. Mean arterial pressure is an average calculated value and gives a better indication of perfusion to vital organs. Pulse pressure is the difference between systolic and diastolic pressure and may be used to assess cardiac function and arterial stiffness.
Analyzing blood pressure measurements requires a comprehensive understanding of normal ranges, recognizing deviations from the norm, and considering the patient’s unique characteristics and medical history. Regular monitoring and collaboration with healthcare professionals ensure accurate interpretation and appropriate management of blood pressure-related concerns.
Evaluating Respiratory Rate
Respiratory rate is a fundamental parameter that measures the number of breaths taken per minute. Evaluating respiratory rate is crucial for assessing a patient’s respiratory function and overall well-being. Let’s explore how to effectively evaluate respiratory rate readings on a vital signs monitor.
The normal range for respiratory rate in adults typically falls between 12 and 20 breaths per minute. However, it is important to consider that respiratory rate can vary depending on various factors, including age, physical activity, pain, anxiety, and underlying medical conditions.
When evaluating respiratory rate readings, it is essential to observe the patient’s breathing pattern, depth, and regularity. Regular breathing refers to breaths that occur at consistent intervals, while irregular breathing may indicate underlying conditions or distress. Additionally, shallow or labored breathing suggests difficulties in efficient respiration.
An increased respiratory rate, known as tachypnea, may indicate factors such as respiratory infections, lung diseases, anxiety, pain, fever, or metabolic disturbances. On the other hand, a decreased respiratory rate, called bradypnea, can result from sedation, certain medications, neurological conditions, or medical emergencies.
It is important to note that respiratory rate alone may not provide a complete picture of respiratory function. Assessing other respiratory parameters, including oxygen saturation levels (SpO2) and the patient’s overall clinical presentation, is crucial for a comprehensive evaluation. Low oxygen saturation levels may indicate inadequate oxygenation, while high oxygen saturation levels may suggest hyperventilation or increased oxygen delivery.
In some cases, a vital signs monitor may also display other respiratory waveforms, such as the capnography waveform or a waveform derived from an arterial blood gas analysis. These waveforms can provide additional insights into the patient’s ventilation, carbon dioxide levels, and acid-base balance. Analyzing these waveforms alongside respiratory rate readings can aid in identifying respiratory abnormalities and guiding appropriate interventions.
Evaluating respiratory rate requires careful observation of the patient’s breathing pattern, depth, and regularity, alongside considering the clinical context and associated parameters such as oxygen saturation levels. Close monitoring and collaboration with healthcare professionals ensure accurate assessment and appropriate management of respiratory conditions.
Assessing Oxygen Saturation Levels
Assessing oxygen saturation levels is a critical aspect of analyzing a patient’s respiratory status and overall oxygenation. Oxygen saturation, often displayed as SpO2 on a vital signs monitor, measures the percentage of hemoglobin in the blood that is carrying oxygen. Let’s explore how to effectively assess oxygen saturation levels and interpret the readings on a vital signs monitor.
A normal oxygen saturation level is typically considered to be 95% or higher. This indicates that the red blood cells are adequately saturated with oxygen, ensuring proper oxygen delivery to the body’s tissues and organs. Oxygen saturation levels below 95% may suggest insufficient oxygenation, known as hypoxemia, which can be a result of various respiratory or cardiovascular conditions.
When assessing oxygen saturation readings, it’s important to consider the patient’s overall clinical presentation and assess any signs or symptoms of respiratory distress, such as shortness of breath or cyanosis (blue tinge to the skin or lips). These can provide additional context and help guide appropriate interventions.
It is worth noting that certain factors can influence oxygen saturation readings. These include low perfusion or poor blood flow to the extremities, peripheral vasoconstriction, cold temperatures, nail polish or artificial nails, and excessive movement during measurement. In such cases, it may be necessary to utilize alternative sites for measurement, such as the earlobe or forehead, to obtain accurate readings.
Understanding the limitations of oxygen saturation readings is crucial. While SpO2 provides valuable information about oxygen levels in the blood, it does not provide insights into the respiratory function or the ability of tissues to utilize oxygen. It is essential to interpret oxygen saturation levels alongside other respiratory parameters, such as respiratory rate and waveform analysis when available, to gain a comprehensive understanding of a patient’s oxygenation status.
Moreover, trends in oxygen saturation levels over time are significant for identifying any progressive changes in a patient’s respiratory condition. Monitoring for sustained or recurring decreases in oxygen saturation can prompt healthcare professionals to intervene promptly and initiate appropriate treatments to optimize oxygenation.
Assessing oxygen saturation levels involves interpreting the SpO2 readings in conjunction with the patient’s clinical presentation, considering potential factors that may affect accuracy, and recognizing trends in oxygen saturation over time. Collaboration with healthcare professionals and utilizing additional respiratory parameters ensures a comprehensive evaluation and appropriate management of oxygenation levels.
Recognizing Abnormalities and Alarms
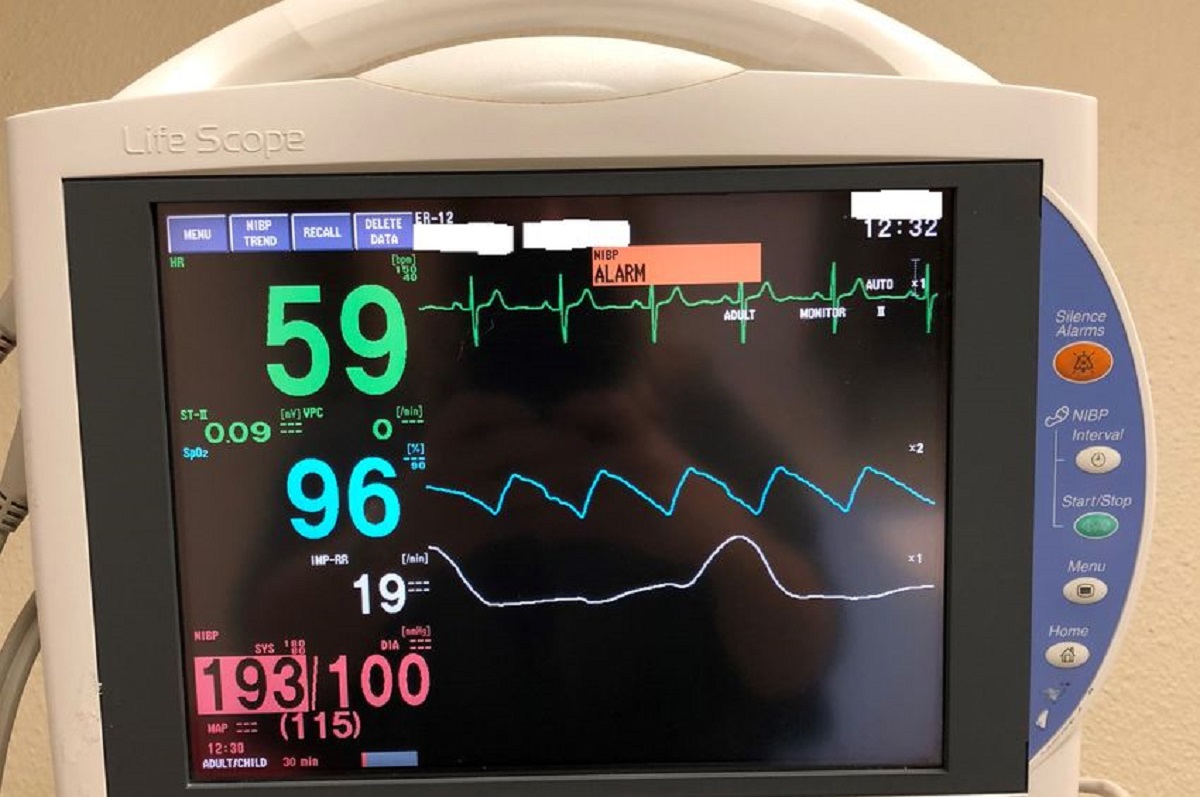
Recognizing abnormalities and responding to alarms on a vital signs monitor is crucial for providing timely and appropriate care to patients. The monitor is designed to alert healthcare professionals to any deviations from normal values or potentially life-threatening situations. Let’s explore how to effectively recognize abnormalities and respond to alarms on a vital signs monitor.
One of the primary functions of a vital signs monitor is to provide real-time updates on physiological parameters such as heart rate, blood pressure, respiratory rate, and oxygen saturation levels. These readings are continuously monitored, and if they exceed preset thresholds or fall outside the established normal ranges, audible and visual alarms are triggered.
When an alarm sounds, it is important to respond promptly and assess the patient’s condition. It’s crucial to differentiate between a genuine alarm indicating a critical situation and false alarms caused by artifact or temporary fluctuations. Careful observation of the patient’s clinical status, as well as considering factors such as movement, dislodged sensors, or faulty equipment, can help determine the appropriate course of action.
Some common alarms encountered on a vital signs monitor include high or low heart rate, abnormal blood pressure readings, high or low respiratory rate, and low oxygen saturation levels. These alarms may signal various underlying issues, such as cardiac arrhythmias, respiratory distress, or inadequate perfusion.
Recognizing abnormal trends or sudden changes in vital signs can be as critical as responding to alarms. Continuous monitoring of trends over time can help identify gradual deteriorations or improvements in a patient’s condition. It is important to regularly assess the patient’s vital signs and compare them to baseline values to detect any significant variations.
Proper response to alarms involves following established protocols and having a clear plan of action. This may involve assessing the patient’s airway, initiating emergency measures, administering medications, or contacting the appropriate healthcare professionals for further assistance.
It must be noted that while vital signs monitors are powerful tools for patient monitoring, healthcare professionals should use their clinical judgment and consider the entire clinical context when responding to alarms. Collaboration with a multidisciplinary team and communication with the patient or their caregivers are also crucial for comprehensive and effective care.
Recognizing abnormalities and responding to alarms on a vital signs monitor require vigilance, clinical judgment, and clear protocols. By remaining attentive to the monitor’s alerts and promptly addressing any potential issues, healthcare professionals can ensure the safety and well-being of their patients.
Troubleshooting Common Issues
Although vital signs monitors are sophisticated medical devices, they can encounter common issues that may affect their accuracy or functionality. Troubleshooting these issues is crucial for ensuring reliable monitoring and accurate measurements. Let’s explore some common problems that can arise with vital signs monitors and how to address them.
1. Sensor Placement: Improper placement of sensors can lead to inaccurate readings. Ensure the sensors are securely attached to the correct anatomical sites as indicated by the manufacturer’s instructions. Proper positioning and adherence to guidelines will help optimize the accuracy of the recorded data.
2. Artifact or Interference: Artifacts or interference can disrupt the signals transmitted from the sensors to the monitor, resulting in distorted readings. Common sources of interference include loose cables, electromagnetic interference from other equipment, or patient movements. Check all connections, secure cables properly, and minimize patient movement to reduce artifacts and ensure accurate measurements.
3. Calibration and Maintenance: Periodic calibration and maintenance are essential for accurate readings. Follow the manufacturer’s guidelines and schedule regular maintenance to ensure that the monitor is properly calibrated and functioning optimally. This includes checking the accuracy of measurements, replacing worn-out components, and updating software as necessary.
4. Power Supply Issues: Power supply problems can disrupt the functioning of vital signs monitors. Ensure the monitor is properly connected to a reliable power source, and check the battery status if operating on battery power. Troubleshoot any power supply issues promptly to prevent interruptions in monitoring.
5. Malfunctioning or Damaged Equipment: Equipment malfunction or physical damage can result in inaccurate readings or complete failure of the monitor. Regularly inspect the vital signs monitor for any signs of damage or malfunction, and address any issues promptly. If necessary, contact the manufacturer for technical support or arrange for repairs.
6. User Error: User error, such as incorrect data entry or incorrect selection of parameters, can lead to misinterpretation of readings. Ensure proper training and familiarization with the specific model of the monitor. Double-check data entry and verify the selected parameters to minimize user error and ensure accurate measurements.
7. Environmental Factors: Environmental factors, such as extreme temperatures, humidity, or inadequate lighting, can impact the performance of vital signs monitors. Follow the manufacturer’s guidelines regarding environmental conditions to ensure optimal functioning of the device. Keep the monitor in a suitable environment and protect it from potential damage.
If troubleshooting steps do not resolve the issue or if there are persistent concerns with the vital signs monitor, it is important to contact the manufacturer’s technical support or a biomedical engineering team for further assistance. They can provide specific guidance and expertise in addressing complex problems or issues that require specialized knowledge.
By being vigilant in troubleshooting common issues, healthcare professionals can ensure that vital signs monitors consistently and accurately provide the necessary information for patient monitoring and care.
Conclusion
Understanding how to read and interpret a vital signs monitor is essential for healthcare professionals and individuals involved in patient care. The ability to accurately assess and analyze vital signs measurements facilitates early detection of abnormalities, enables prompt intervention, and enhances patient outcomes. Throughout this article, we explored the basics of a vital signs monitor, including heart rate, blood pressure, respiratory rate, and oxygen saturation levels.
We discussed the importance of understanding normal ranges, recognizing deviations, and considering the patient’s clinical presentation when interpreting readings. We also emphasized the significance of trends in vital signs over time, identifying abnormalities, and responding to alarms promptly. Additionally, troubleshooting common issues that may occur with vital signs monitors is crucial for ensuring accurate measurements and reliable monitoring.
It’s important to note that while this guide provides valuable insights into reading and interpreting vital signs measurements, it is essential to rely on clinical judgment, consult healthcare professionals, and undergo proper medical training for accurate assessment and treatment. The information presented here serves as a foundation of knowledge, but it is not a substitute for professional expertise.
By mastering the art of reading vital signs monitors, healthcare professionals can provide timely and effective care, monitor patients’ progress, and make informed decisions based on the collected data. Whether in hospitals, clinics, or other healthcare settings, accurate interpretation of vital signs readings is a fundamental skill that contributes to improving patient outcomes and quality of care.
Continued education and staying up-to-date with advancements in vital signs monitoring technology will further enhance our understanding and interpretation of these vital parameters. By integrating our expertise with the capabilities of vital signs monitors, we can provide more comprehensive and personalized care to patients.
So, embrace the knowledge you have gained and be confident in your ability to read and interpret vital signs monitors. By doing so, you are contributing to the well-being and health of those under your care. Stay curious, be vigilant, and continue to learn, as the field of vital signs monitoring evolves and new discoveries are made.