Introduction
Living with diabetes can be a challenging and demanding experience. The constant need to monitor blood glucose levels, manage insulin administration, and make lifestyle adjustments can cause stress and disrupt daily routines. Fortunately, advancements in technology have greatly improved diabetes management, giving individuals more control and flexibility in their daily lives. One such advancement is the continuous glucose monitor (CGM), a device that has revolutionized how blood glucose levels are monitored and managed.
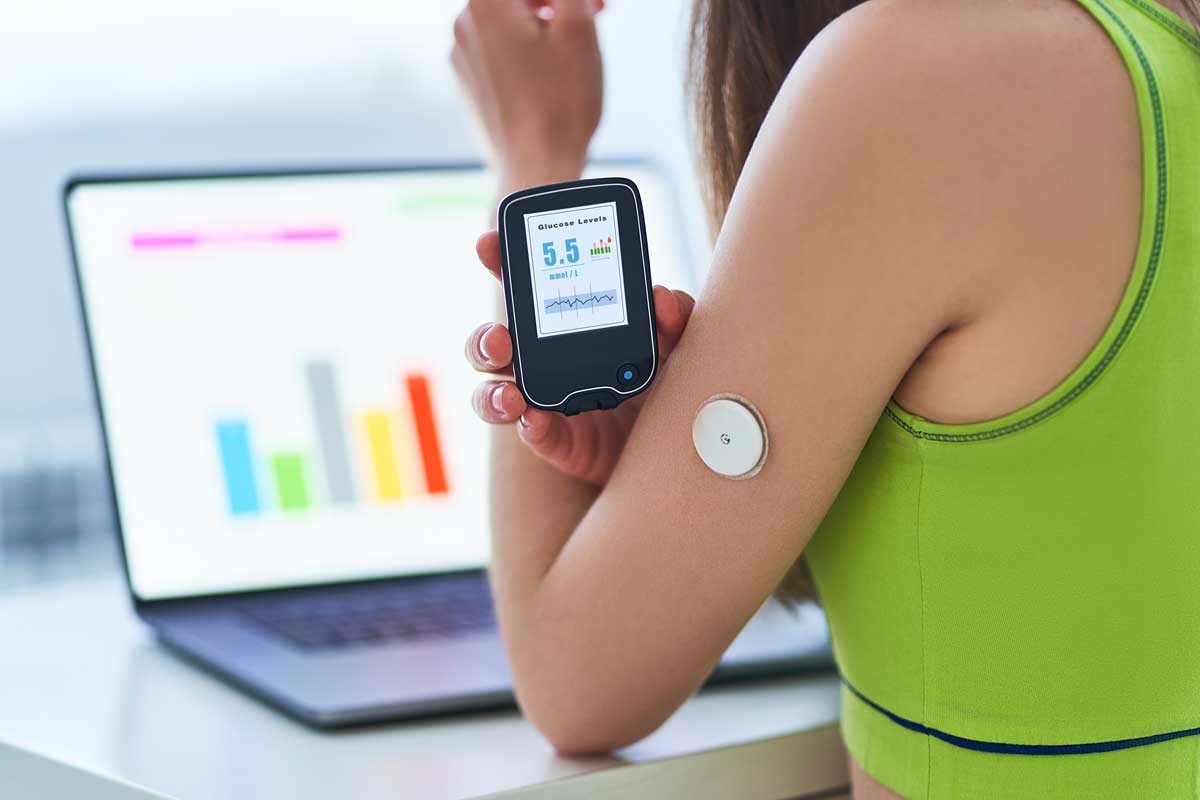
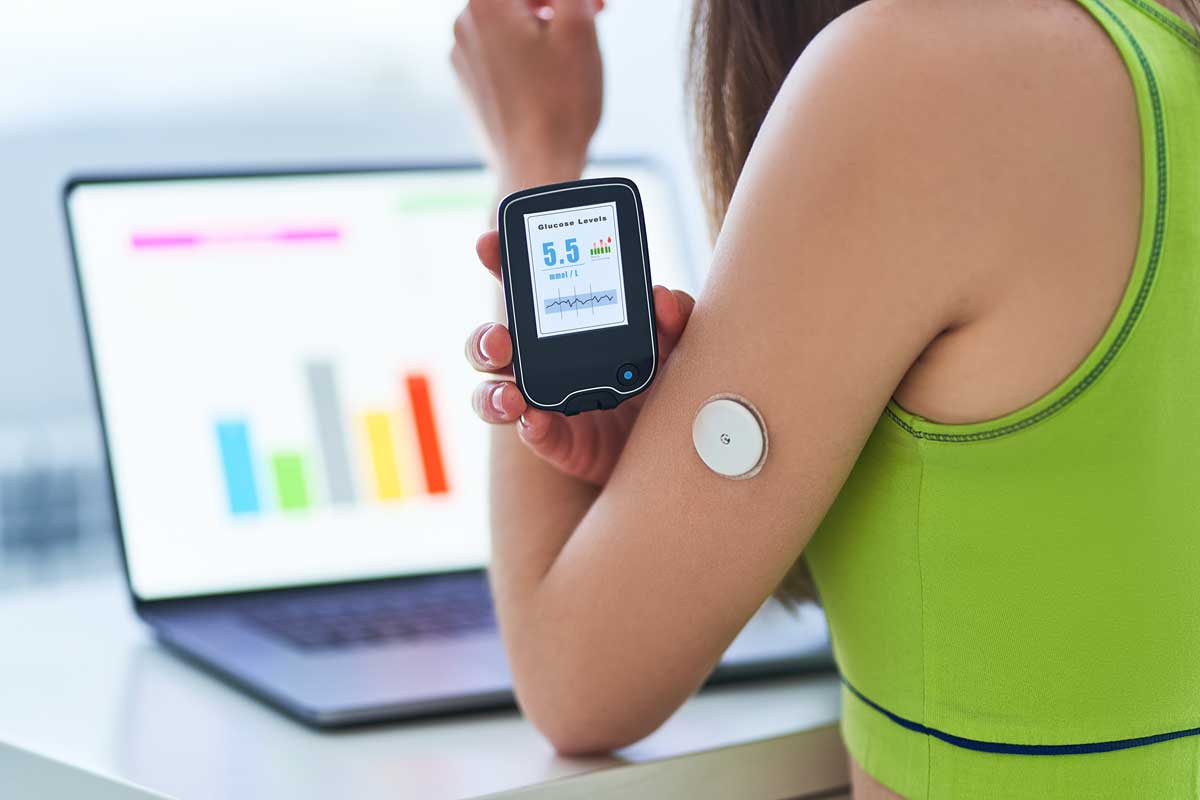
A continuous glucose monitor, or CGM, is a small electronic device that tracks blood glucose levels throughout the day and night. It provides real-time data about glucose levels, allowing individuals to make informed decisions about their diabetes management. CGMs have gained immense popularity among people with diabetes because they offer many benefits and advantages over traditional blood glucose monitoring methods.
CGMs consist of three main components: a small sensor that is inserted under the skin to measure glucose levels, a transmitter that wirelessly transmits glucose data to a receiver or smartphone, and a receiver or smartphone app that displays and analyzes the glucose data. This technology has transformed the way diabetes is managed by providing continuous and convenient access to glucose readings, helping individuals understand their glucose patterns, and allowing for proactive and timely interventions.
In this article, we will explore how CGMs work, the different components of a CGM system, and the various features and functionalities they offer. We will also delve into the benefits of using a CGM and how the data provided by a CGM can be used to optimize diabetes management. Whether you are considering using a CGM or simply curious about how these devices function, this article will provide you with a comprehensive understanding of how CGMs work and the value they bring to individuals managing diabetes.
What is a Continuous Glucose Monitor (CGM)?
A continuous glucose monitor (CGM) is a small electronic device that measures glucose levels in real-time throughout the day and night. It is designed to provide individuals with diabetes with a consistent, user-friendly, and reliable tool for monitoring blood glucose levels.
Unlike traditional blood glucose monitoring methods, which require manual finger pricks and provide discrete glucose readings at specific moments, CGMs offer a continuous stream of glucose data. This constant monitoring allows individuals to have a better understanding of their glucose trends, patterns, and variability, helping them make informed decisions about their diabetes management.
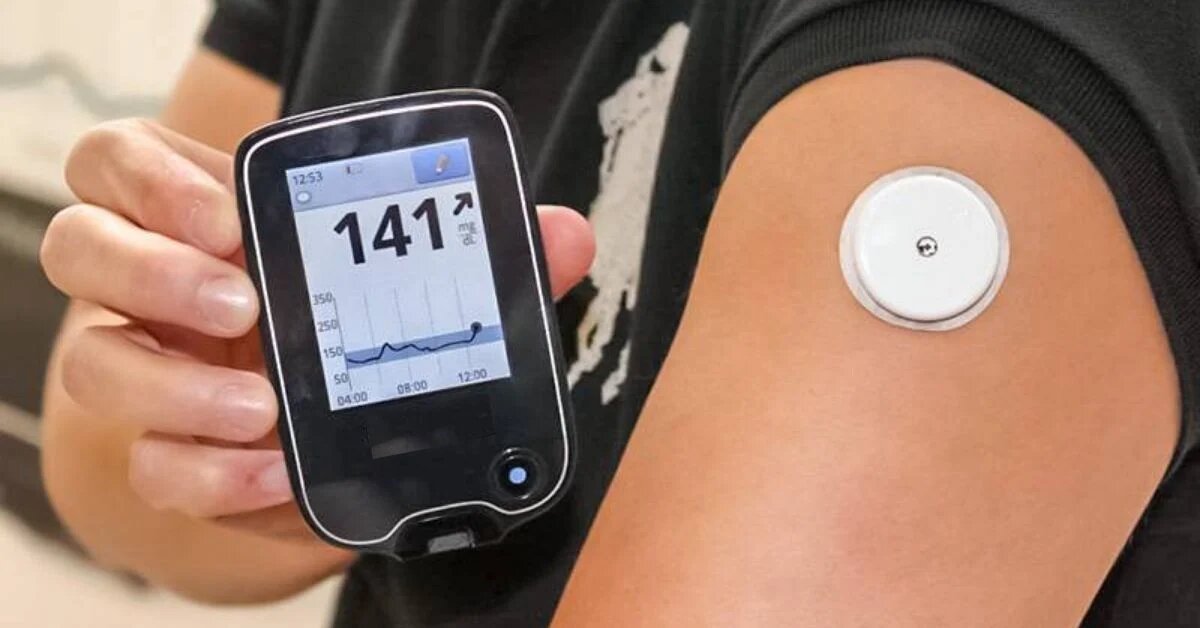
The main component of a CGM is a small sensor that is inserted under the skin, usually on the abdomen or arm. This sensor measures the glucose levels in the interstitial fluid surrounding the cells and converts this data into glucose readings. The sensor is connected to a transmitter, which wirelessly transmits the glucose data to a receiver or a smartphone app.
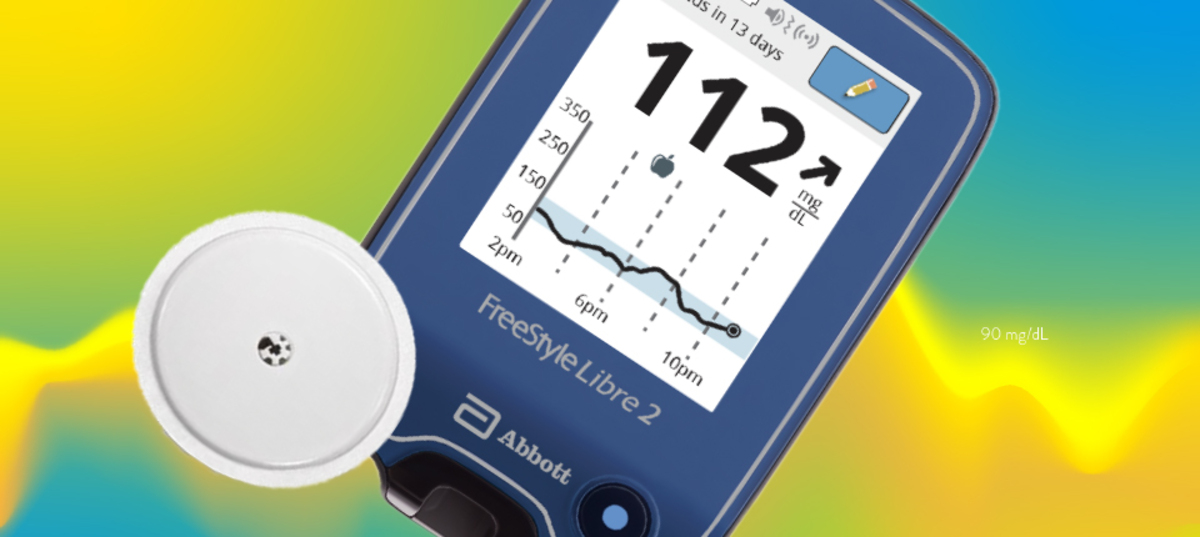
The receiver or smartphone app displays the glucose readings in an easy-to-understand format, usually in the form of real-time graphs, charts, and numerical values. Some CGMs also provide color-coded alarms and alerts to notify users of hypo- or hyperglycemic events, helping them take immediate action to prevent complications.
CGMs are compatible with insulin pumps and can be integrated into closed-loop systems, also known as artificial pancreas systems. These systems automate insulin delivery based on the CGM data, providing a more precise and personalized approach to diabetes management.
It is important to note that CGM readings may slightly lag behind the actual blood glucose levels due to the time it takes for glucose to travel from the blood vessels to the interstitial fluid. However, CGMs still offer a significant improvement in the frequency and convenience of glucose monitoring compared to traditional methods.
Overall, CGMs have revolutionized the way blood glucose is monitored and managed, offering individuals with diabetes greater insight and control over their condition. By continuously tracking glucose levels, CGMs enable proactive decision-making, help identify trends and patterns, and empower individuals to make necessary adjustments to their lifestyle, medication, and insulin dosing to achieve optimal diabetes management.
Benefits of Using a CGM
The use of a continuous glucose monitor (CGM) offers a range of benefits for individuals managing diabetes. Let’s explore some of the key advantages of using a CGM:
- Real-time visibility: One of the primary benefits of a CGM is the ability to monitor glucose levels in real-time. CGMs provide continuous updates on glucose readings, allowing individuals to see how their glucose levels change throughout the day. This real-time visibility helps users make immediate and informed decisions regarding their diabetes management.
- Trend identification: CGMs display glucose data using visual graphs and charts. This enables users to identify trends and patterns in their glucose levels over time. By analyzing these patterns, individuals can gain insights into how their body responds to different foods, activities, and medications, enabling them to make necessary adjustments for better glucose control.
- Early detection of highs and lows: CGMs provide alerts and alarms when glucose levels go above or below a certain threshold. These alerts can help individuals detect and respond to hypoglycemic (low blood sugar) or hyperglycemic (high blood sugar) events sooner, reducing the risk of complications and allowing for prompt intervention.
- Reduced finger pricks: Unlike traditional blood glucose monitoring methods, which require frequent finger pricks throughout the day, CGMs reduce the need for manual testing. Although periodic finger pricks are still necessary for calibrating the CGM and confirming accuracy, the frequency of finger pricks is significantly reduced, making glucose monitoring less invasive and more convenient.
- Improved quality of life: CGMs offer individuals with diabetes greater freedom and flexibility in managing their condition. With continuous glucose monitoring, users can confidently engage in daily activities, exercise, and social events, knowing that they have better control over their blood glucose levels. This improved quality of life can lead to reduced stress and anxiety surrounding diabetes management.
- Integration with insulin pumps and closed-loop systems: CGMs can be seamlessly integrated with insulin pumps and closed-loop systems, allowing for automated insulin delivery based on real-time glucose data. By connecting these technologies, individuals can achieve tighter glucose control and minimize the risk of hypoglycemia or hyperglycemia.
By utilizing a CGM, individuals can gain valuable insights into their glucose levels, optimize their diabetes management, and ultimately improve their overall health and well-being. The benefits of using a CGM extend beyond glucose monitoring, offering individuals more control, convenience, and peace of mind in their diabetes journey.
Components of a CGM System
A continuous glucose monitor (CGM) system consists of several essential components that work together to provide individuals with diabetes with accurate and continuous glucose data. Let’s take a closer look at the main components of a CGM system:
- Sensor: The sensor is a tiny, flexible component that is inserted under the skin to measure glucose levels in the interstitial fluid. It typically consists of a thin, flexible wire with a glucose-sensing electrode at the tip. The sensor collects glucose measurements and sends the data to the transmitter.
- Transmitter: The transmitter is a small device that is connected to the sensor. It is responsible for wirelessly transmitting the glucose readings from the sensor to either a receiver or a smartphone app. The transmitter uses Bluetooth technology or other wireless communication methods to ensure seamless data transmission.
- Receiver: The receiver is a handheld device or a dedicated device that displays the glucose readings provided by the CGM system. It receives the transmitted data from the transmitter and presents it to the user in a user-friendly format, such as graphs, charts, or numerical values. Some CGM systems require a separate receiver, while others can use a smartphone app as the receiver.
- Smartphone App: Many CGM systems offer companion smartphone apps that can function as the receiver. These apps allow users to view and analyze their glucose data directly on their smartphones. The apps often provide additional features, such as trend analysis, data sharing, and integration with other health and fitness apps.
- Calibration: Calibration is the process of aligning the CGM system’s readings with a traditional blood glucose meter. Calibration typically involves performing a finger prick test and entering the corresponding blood glucose value into the CGM system. This helps improve the accuracy of the CGM readings, as interstitial fluid glucose measurements may lag behind actual blood glucose levels.
- Alarms and Alerts: CGM systems often include customizable alarm and alert features that notify users of potentially high or low glucose levels. Users can set thresholds for these alerts based on their personal glucose targets. When glucose levels exceed or fall below these thresholds, the CGM system will provide visual, audible, or vibrating alarms to prompt the user to take necessary action.
It is important to note that the specific components of a CGM system may vary depending on the brand and model. Some CGM systems may have additional features, such as trend prediction algorithms, advanced data analytics, or integration with insulin pumps or closed-loop systems.
By understanding the different components of a CGM system, individuals can make an informed decision when choosing a CGM that aligns with their needs and preferences. Each component plays a vital role in ensuring accurate and continuous glucose monitoring, empowering individuals to take control of their diabetes management.
How Does a CGM Work?
A continuous glucose monitor (CGM) works by utilizing advanced technology to continuously measure and monitor glucose levels in individuals with diabetes. Let’s explore the process of how a CGM works:
1. Insertion of the Sensor: The CGM system begins with the insertion of a small sensor under the skin. The sensor is typically placed on the abdomen or arm, and it contains a tiny electrode that measures glucose levels in the interstitial fluid surrounding the cells.
2. Glucose Measurement: Once inserted, the sensor starts collecting glucose measurements. It measures the glucose levels in the interstitial fluid by detecting the glucose oxidase reaction, which converts glucose into hydrogen peroxide. The sensor then converts this reaction into an electrical signal proportional to the glucose concentration.
3. Data Transmission: The sensor is connected to a transmitter, which wirelessly transmits the glucose data to either a receiver or a smartphone app. The transmitter uses Bluetooth or other wireless communication technology to ensure seamless data transmission.
4. Glucose Data Display: The receiver or smartphone app receives the transmitted data and presents it to the user in a user-friendly format. Typically, the glucose readings are displayed as real-time graphs, charts, or numerical values, allowing users to monitor their glucose levels continuously throughout the day.
5. Continuous Monitoring: The CGM system constantly collects and updates the glucose readings, providing users with continuous monitoring of their glucose levels. Users can see how their glucose levels change in response to meals, physical activity, and insulin administration, helping them make informed decisions about their diabetes management.
6. Data Analysis and Trend Identification: CGM systems often include advanced data analysis capabilities, allowing users to identify trends and patterns in their glucose levels over time. By analyzing these trends, individuals can gain insights into how their body responds to various factors and make necessary adjustments to their diabetes management.
7. Alerts and Alarms: CGM systems have customizable alert and alarm features that notify users of potentially high or low glucose levels. Users can set their target glucose range, and when glucose levels exceed or fall below these thresholds, the CGM system will provide visual, audible, or vibrating alarms to prompt the user to take necessary action.
It is important to note that CGM readings may lag slightly behind actual blood glucose levels due to the time it takes for glucose to travel from the blood vessels to the interstitial fluid. However, CGMs still provide valuable and continuous information about glucose levels, empowering individuals to stay in control of their diabetes management.
Overall, CGMs enable individuals with diabetes to have a better understanding of their glucose levels in real time. By providing continuous monitoring, data analysis, and alert features, CGM systems contribute to improved glucose control and better diabetes management.
Sensor Placement and Calibration
Proper sensor placement and calibration are crucial for the accurate and reliable functioning of a continuous glucose monitor (CGM). Let’s delve into the importance of sensor placement and calibration in CGM systems:
Sensor Placement: The sensor is a vital component of the CGM system as it measures glucose levels in the interstitial fluid. It is essential to follow the manufacturer’s instructions for sensor placement to ensure accurate readings. Common insertion sites include the abdomen or arm, but specific recommendations may vary depending on the CGM system. Cleanliness is key, so thoroughly clean the insertion site before attaching the sensor to minimize the risk of infection. Proper insertion technique and site rotation can prevent discomfort and irritation, ensuring the sensor remains secure during wear.
Calibration: Calibration is the process by which a CGM system is aligned with traditional blood glucose meter readings. Regular calibration helps improve the accuracy of CGM readings. Calibration typically entails performing a finger prick test using a blood glucose meter and inputting the corresponding value into the CGM system. The frequency of calibration may vary depending on the manufacturer’s recommendations, but it is typically required at least twice a day and when the CGM readings are not consistent with how an individual feels. Accurate calibration allows the CGM system to adjust and refine its glucose measurements, providing reliable and informative data.
During calibration, it is important to ensure that the blood glucose meter used for calibration is accurate and properly maintained. Using control solutions provided by the manufacturer can help verify the accuracy of the blood glucose meter. Additionally, follow the manufacturer’s instructions for entering the calibration value into the CGM system, as inaccurate or incorrect input can lead to misleading glucose readings.
It is essential to note that CGM readings may slightly differ from blood glucose meter readings due to several factors, including the lag time between blood glucose changes and interstitial fluid glucose changes. This difference is known as the sensor lag. Calibration helps minimize this discrepancy and fine-tune the CGM system’s measurements. However, it’s important to remember that CGM readings are not intended to replace fingerstick glucose measurements entirely and should be used in conjunction with regular blood glucose monitoring for accurate diabetes management.
Individuals should closely follow the manufacturer’s instructions regarding sensor placement and calibration specific to their CGM system. Proper sensor placement and calibration practices result in accurate and reliable glucose readings, helping individuals make informed decisions about their diabetes management, such as adjusting insulin doses, managing dietary choices, and timing physical activity. By ensuring correct sensor placement and timely calibration, individuals can optimize the performance of their CGM system and derive the maximum benefit from this innovative technology.
Data Interpretation and Analysis
Continuous glucose monitoring (CGM) systems provide individuals with diabetes a wealth of glucose data that requires interpretation and analysis to derive meaningful insights. Let’s explore how data interpretation and analysis play a crucial role in optimizing diabetes management:
Visual Representation: CGM systems present glucose data in various visual formats, such as real-time graphs, charts, and numerical values. These visual representations allow users to visualize trends and fluctuations in their glucose levels over time. By observing patterns, spikes, or dips, individuals can identify factors that affect their glucose control, such as meals, exercise, stress, or medication timing.
Trend Identification: Trend identification involves analyzing the patterns and trends displayed in the CGM data. Users can detect recurring patterns in glucose levels, such as post-meal spikes, overnight drops, or specific time-of-day variations. Recognizing these trends enables individuals to make proactive adjustments to their diabetes management, such as adjusting insulin doses, modifying meal plans, or planning exercise activities strategically.
Time in Range: Time in Range (TIR) is a key metric used in CGM analysis. It refers to the amount of time spent within a target glucose range, typically defined by healthcare professionals. CGM systems can calculate TIR and display the percentage of time spent in range. Aiming for a higher TIR percentage indicates better glucose control and can serve as a goal to strive for in diabetes management.
Hypoglycemia and Hyperglycemia Analysis: CGM data analysis allows for the identification of episodes of hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar). By reviewing the data, users can pinpoint the frequency, duration, and potential triggers of these events. This information helps individuals take preventive measures to reduce the risk of hypoglycemic or hyperglycemic episodes, such as adjusting insulin dosing, timing meals or snacks, or modifying exercise routines.
Data Sharing: Many CGM systems offer the option to share data with healthcare providers or family members. Data sharing facilitates collaborative decision-making and enables healthcare professionals to provide personalized recommendations. Sharing CGM data with healthcare providers allows for remote monitoring, reducing the need for regular in-person visits and facilitating timely adjustments to treatment plans.
Integration with Other Health Data: CGM systems can integrate with other health-related data, such as food intake, exercise, and insulin dosing. This integration provides a holistic view of an individual’s diabetes management. By correlating glucose data with these factors, users can evaluate their impact on glucose control and optimize lifestyle choices accordingly.
Data interpretation and analysis play a vital role in transforming raw glucose data into actionable information. By leveraging the insights gained from CGM data analysis, individuals can make informed decisions, personalize their diabetes management, and achieve better glucose control. Regular review and analysis of CGM data enable individuals to gain a deeper understanding of their condition and make appropriate adjustments to their diabetes management plan with the aim of improving overall health and well-being.
Alert and Alarm Features
Continuous glucose monitoring (CGM) systems are equipped with alert and alarm features to notify individuals with diabetes of critical changes in their blood glucose levels. These features serve as important tools for proactive management and prevention of potentially dangerous situations. Let’s dive into the alert and alarm features of CGM systems:
Low Glucose Alerts: CGM systems can be programmed to provide alerts when blood glucose levels drop below a certain threshold. These low glucose alerts, also known as hypoglycemic alerts, are important for timely intervention to prevent severe hypoglycemia. Users can set their personalized low glucose threshold based on their specific needs and healthcare professional’s recommendations. When the CGM system senses that blood glucose levels are approaching or have reached the low glucose threshold, it triggers an alert to signal the need for immediate action, such as consuming a fast-acting source of carbohydrates.
High Glucose Alerts: High glucose alerts, or hyperglycemic alerts, notify individuals when blood glucose levels rise above a specified threshold. These alerts help individuals take appropriate measures, such as adjusting insulin dosing or making dietary modifications, to prevent prolonged hyperglycemia and related complications. By setting a personalized high glucose threshold, CGM systems trigger alarms and alerts when blood glucose levels exceed the set limit, prompting users to take corrective actions to bring their glucose levels back into the target range.
Rate of Change Alerts: Rate of change alerts in CGM systems notify users when their glucose levels are increasing or decreasing too rapidly. These alerts indicate sudden spikes or drops in glucose levels and allow individuals to address these rapid changes promptly. The rate of change alerts provides valuable information about glucose variability and helps users identify triggers or patterns that might be contributing to unstable blood glucose control.
Customizable Alarms: CGM systems often offer customizable alarms that allow users to set specific thresholds for alerts based on their individual glucose targets. Users can customize the timing, sound, or vibration level of the alarms to suit their preferences and accommodate their lifestyles. Customizable alarms enable individuals to adapt the CGM system to their unique needs and ensure they receive alerts at critical glucose levels without excessive or unnecessary notifications.
Snooze and Override Features: CGM systems may provide snooze and override options for alerts and alarms. Snooze functions allow users to temporarily silence or delay the alerts when they need a short interruption or more time to address the situation. Override features allow users to acknowledge and dismiss alerts if they determine that the glucose reading is accurate and the alert is unnecessary. These features provide flexibility and control over the alert system, empowering individuals to manage their CGM according to their specific circumstances.
Alert and alarm features in CGM systems contribute to improved glucose management and enhanced safety for individuals with diabetes. By promptly notifying users of critical changes in their blood glucose levels, CGM systems enable proactive intervention to prevent severe hypoglycemia, address hyperglycemia, and maintain glucose control within target ranges. These features, when utilized effectively, provide peace of mind and assist in minimizing risks associated with diabetes-related complications.
Using CGM Data for Diabetes Management
The data provided by continuous glucose monitoring (CGM) systems is a powerful tool that individuals with diabetes can utilize to optimize their diabetes management strategies. Let’s explore how CGM data can be effectively utilized for diabetes management:
Real-Time Monitoring: CGM data allows individuals to monitor their glucose levels in real-time. This real-time monitoring provides insight into how different factors, such as meals, physical activity, stress, and medication, affect glucose levels throughout the day. By observing these patterns and trends, users can make immediate adjustments to their diabetes management strategy, such as adjusting insulin doses, eating specific foods, or engaging in exercise to maintain glucose control within target ranges.
Trend Analysis: CGM systems provide visual representations of glucose data, allowing users to analyze trends over an extended period. By examining these trends, individuals can identify patterns that impact their glucose control, such as consistent post-meal spikes or recurrent hypoglycemic episodes during exercise. This trend analysis can guide personalized interventions, such as modifying meal plans or adjusting medication timing, to achieve better glucose stability and control.
Time in Range (TIR): TIR is a key metric derived from CGM data that indicates the amount of time spent within a target glucose range. Users can set their desired target range in collaboration with healthcare professionals. Monitoring TIR provides a snapshot of overall glycemic control, with higher percentages of time spent in range correlating with better outcomes. Analyzing TIR encourages individuals to aim for improved glucose stability and helps them evaluate the effectiveness of their diabetes management strategies.
Hypoglycemia and Hyperglycemia Management: CGM data allows early detection of hypoglycemic (low blood sugar) and hyperglycemic (high blood sugar) episodes. CGM systems provide alerts or alarms when glucose levels fall or rise beyond set thresholds, enabling individuals to take prompt action. By closely monitoring and analyzing hypoglycemic and hyperglycemic events, users can identify triggers and implement preventive measures, such as adjusting medication doses, timing of meals or snacks, or modifying exercise routines to minimize the occurrence of these events.
Data Sharing with Healthcare Professionals: CGM systems often have the capability to share glucose data with healthcare professionals, facilitating collaborative decision-making. By sharing CGM data with healthcare providers, individuals receive valuable guidance and personalized recommendations for managing their diabetes. Healthcare professionals can evaluate the data, identify areas of concern, provide tailored advice, and make adjustments to treatment plans remotely, reducing the need for frequent in-person visits.
Integration with Other Health Data: CGM systems can be integrated with other health-related data, such as food and exercise logs, insulin dosing records, and sleep patterns. This integration allows for a comprehensive view of an individual’s diabetes management. By correlating glucose data with these factors, users can identify causal relationships, assess the impact of lifestyle choices, and make informed decisions regarding nutrition, exercise, and medication adjustments for optimal glucose control.
The use of CGM data empowers individuals with diabetes to make informed decisions and take proactive steps towards managing their condition effectively. By utilizing real-time data monitoring, personalized trend analysis, and targeted interventions, individuals can aim for improved glucose stability, reduce the risk of complications, and ultimately enhance their overall health and well-being.
Tips for Successful CGM Use
Using a continuous glucose monitor (CGM) effectively can enhance diabetes management and maximize the benefits of this technology. Here are some tips to ensure successful CGM use:
1. Familiarize Yourself with the Device: Take the time to thoroughly read the user manual and become familiar with the functions and capabilities of your CGM system. Understand how to interpret glucose data, set alarms, calibrate the device, and troubleshoot any issues that may arise.
2. Proper Sensor Placement: Follow the manufacturer’s instructions for sensor placement to ensure accurate readings. Cleanse the insertion site with an alcohol wipe and allow it to dry before inserting the sensor. Rotate insertion sites to prevent irritation or discomfort, and monitor for any signs of infection or skin issues.
3. Regular Calibration: Calibration is essential for accuracy. Follow the recommended calibration schedule provided by the manufacturer and calibrate when blood glucose levels are stable. Avoid calibrating during times of rapid glucose fluctuation, such as immediately after a meal or exercise.
4. Use Trend Data to Inform Decision-Making: Analyze the trend data from your CGM to identify patterns and make informed decisions about your diabetes management. Look for recurring high or low points, recognize how certain foods or activities affect your glucose levels, and adjust your treatment plan accordingly.
5. Set Personalized Alarms and Alerts: Customize the alarm settings on your CGM to fit your individual needs and preferences. Set personalized low glucose and high glucose thresholds that align with your target ranges, and adjust alarm volume or vibration to ensure you will notice important alerts without unnecessary interruptions.
6. Communicate with Your Healthcare Team: Regularly share CGM data with your healthcare team, including trends, patterns, and any concerns you may have. Collaborate with your healthcare provider to make adjustments to your diabetes management plan based on the insights gained from your CGM data.
7. Avoid Overreliance on CGM Data: While CGM data is valuable, it’s essential to remember that it is just one tool in your diabetes management toolkit. Use CGM data in conjunction with fingerstick blood glucose measurements and clinical assessments to ensure accurate and reliable glucose control.
8. Stay Hydrated: Maintaining proper hydration is important for accurate CGM readings. Drink enough water throughout the day to ensure adequate interstitial fluid levels, which can positively impact the accuracy of glucose readings.
9. Ensure Sensor Adhesion: Properly secure the CGM sensor to ensure it stays in place during daily activities. Follow the manufacturer’s recommendations for adhesion, such as using adhesive patches or skin prep wipes, to maintain sensor integrity.
10. Take Advantage of CGM Education and Support: Seek educational resources and support from diabetes educators, online communities, and CGM manufacturers. Attend training sessions, webinars, or workshops to learn more about CGM technology and how to make the most of your device.
By following these tips, individuals can optimize their CGM experience and use the data provided by their device to make informed decisions, improve glucose control, and enhance their overall diabetes management.
Conclusion
Continuous glucose monitoring (CGM) systems have transformed diabetes management by providing individuals with real-time and continuous access to their glucose data. These advanced devices offer numerous benefits, including real-time visibility into glucose levels, trend analysis, and the early detection of hypoglycemia and hyperglycemia. By utilizing the data and features provided by CGM systems, individuals with diabetes can make proactive decisions, optimize their diabetes management strategies, and improve their overall well-being.
Through proper sensor placement, regular calibration, and a thorough understanding of how to interpret CGM data, individuals can maximize the accuracy and reliability of their CGM system. Personalized alarms and alerts, along with trend analysis, allow users to identify glucose patterns and take swift action to maintain glucose control within target ranges.
Sharing CGM data with healthcare professionals fosters collaborative decision-making, fine-tuning diabetes management plans, and ensuring personalized recommendations. Integration with other health data enables a holistic view of an individual’s diabetes management, fostering a comprehensive understanding of factors influencing glucose control.
Successful CGM use requires a balanced approach, acknowledging the importance of CGM data while remembering to complement it with fingerstick blood glucose measurements and clinical assessments. It’s essential to stay hydrated, ensure proper sensor adhesion, and remain engaged in CGM education and support opportunities.
Overall, CGM systems empower individuals with diabetes to take control of their condition, make proactive choices, and optimize their diabetes management. By leveraging the continuous and accurate glucose data provided by CGM devices, individuals can achieve better glucose control, decrease the risk of complications, and enhance their overall quality of life.